MOTIVATION
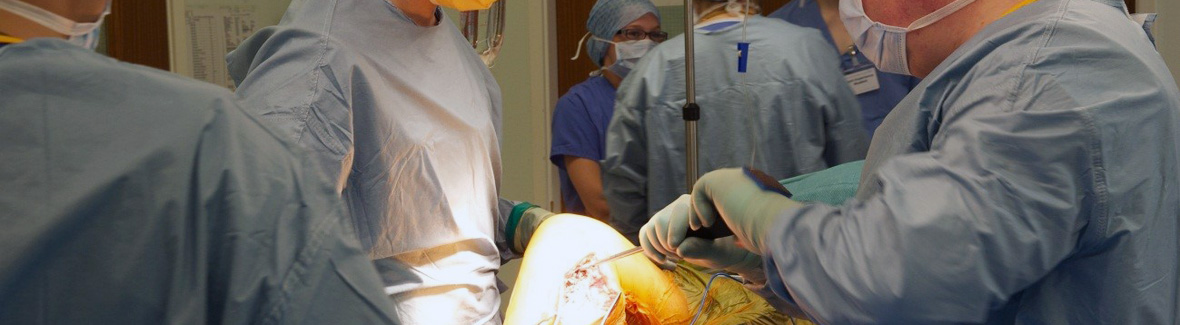
Osteoarthritis (OA) is one of the most prevalent chronic conditions as identified in Bone & Joint Decade. According to the World Health Organisation, 40% of people over 70 years old have OA. This joint disease affects around 0.4 billion people’s life, with patients in Europe accounting for up to 30%. The figure is set to increase with the ageing problem. Patients with OA often suffer pain, loss of mobility and go on to require an end stage total joint replacement. This will happen when the loss of quality of cartilage and bone at the joint interface has significantly reduced the quality of life of the patient, and non-surgical treatments are no longer effective.
The current state of the art in terms of medically necessary surgical intervention of large cartilaginous defects (>1.5 cm2) is autologous chondrocyte implantation (ACI). In this surgical procedure the associated costs and infection are the main concern. For small osteochondral defects, microfracture (MF) marrow stimulation is considered medically necessary treatment. However, MF produces fibrocartilage not native hyaline cartilage.
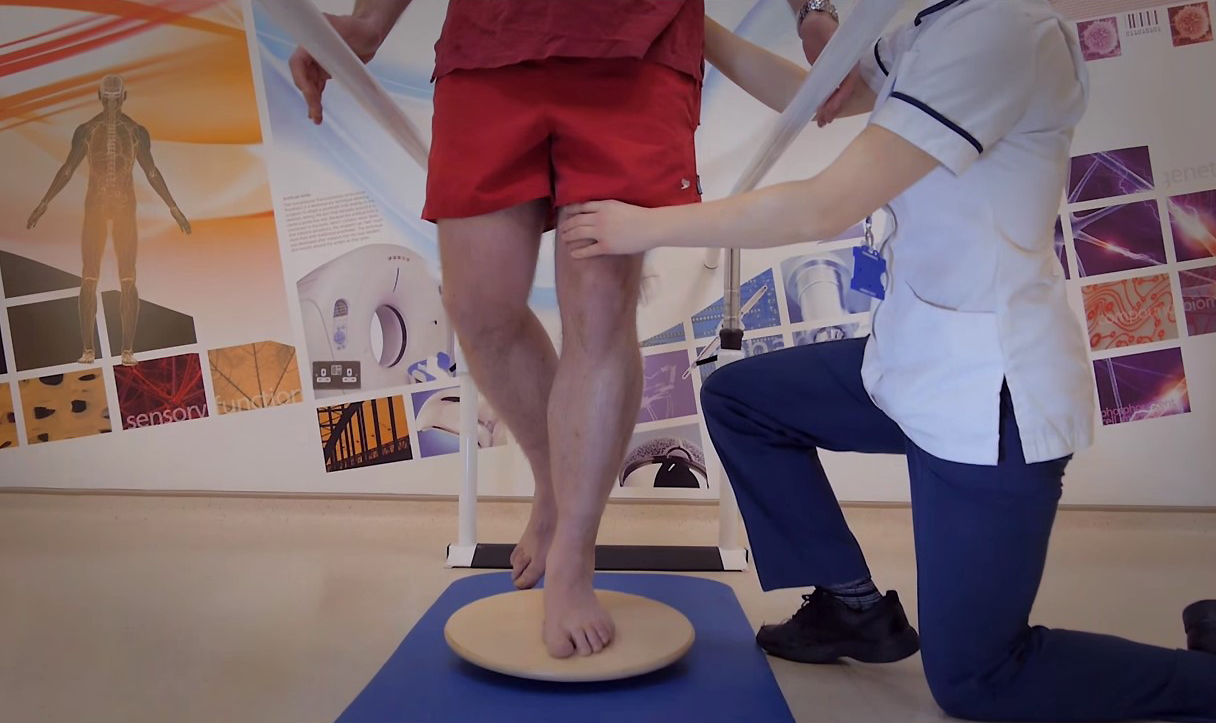
Treatments using tissue engineering methods have been established and are promising for the treatment of small osteochondral defects. In this approach, the use of 3D scaffolds (with or without cells) has been used to provide support for tissue growth. Commercially available scaffolds have been used for the treatment of these small cartilage and osteochondral defects (<1.5 cm2). However, none of these products promote satisfactory durable regeneration of large osteochondral defects.
In order to address this challenge, the project BAMOS bring together five internationally leading research organisations, one healthcare providers and one company working in additive manufacturing, who will undertake complementary and coordinated projects in order to collaborate on the development, manufacturing and marketing of the osteochondral scaffold that will bridge the gap between small osteochondral defect treatment and joint replacement.